.
Feb. 23, 2017
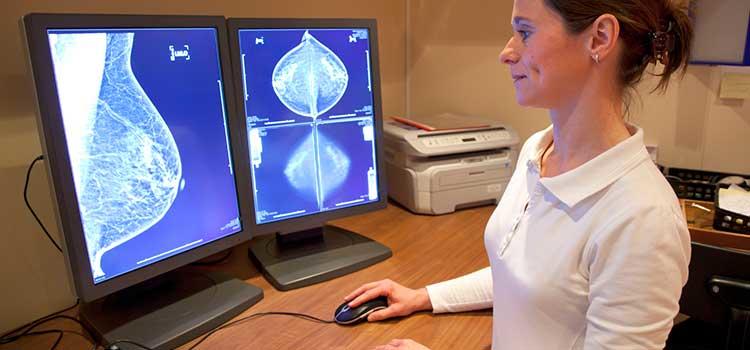
Traditionally, x-ray, MRI and ultrasound are used in breast imaging. Dr. Elise Fear, PhD, professor in electrical and computer engineering at UCalgary’s Schulich School of Engineering, is pioneering the use of microwave technology to complement those diagnostic tools.
“Microwaves have different interactions with tissue based on water content,” she says. “Fat tissue has more water than glandular tissue, so using microwave imaging we can come up with information on the structure of the breast.” This, in conjunction with the traditional imaging methods, provides details about a patient’s breast health that might not otherwise be available.
After lumpectomy surgery – where a portion of the breast is removed – and radiation treatment, patients can sometimes develop scar tissue. “As well as the discomfort this can cause, there can be an impact on cosmetic results,” explains Fear. “With microwave imaging we may be able to detect and monitor these side effects. Long term, this may give us the ability to align the treatment to the patient.”

.
The microwaves used are much less powerful than what you use with a cellphone, Fear says. “When we talk about microwaving people, we are not heating them up.”
“When we talk about microwaving people, we are not heating them up.”
The larger of the two scanners Fear uses for her research involves zero breast compression, something most women will see as a huge advantage. Instead, the volunteer lies on her stomach on the table-sized scanner, which has a hole for the breast to go through. It dips into a container of canola oil, which acts somewhat like the gel used in ultrasound imaging. The oil holds microwave antennas, lasers and a camera to create the breast image.
“We’ve done about 25 scans of volunteers so far, and one of the reasons we’ve done so few is that it takes about half an hour per breast to do the scan. MR scans take about 45 minutes for both breasts, so it’s not an unreasonable amount of time,” says Fear.
The second scanner is small enough that it can fit on a cart, making it easy to take to the Foothills Hospital. There, it takes just five minutes to scan both breasts.
While not a commercially available technology – yet – Fear hopes to scan approximately 100 volunteers and have a clear picture of its clinical potential in three to five years.
Diagnose the undiagnosable. Treat the untreatable. Solve the unsolvable.
Advances in genomics – the study of genes and their functions – will allow researchers and eventually physicians to customize health care and treat individuals according to their genetic makeup. This “precision medicine” approach will give physicians more tools to understand what their patients need, and to provide highly personalized, precise care, says Francois Bernier.
Dr. Bernier, a member of the Alberta Children's Hospital Research Institute, is the head of the department of medical genetics at the Cumming School of Medicine and director of the clinical genetics unit at the Alberta Children’s Hospital. He speaks with enthusiasm about the advances that have been made possible with the ability to sequence a person’s genome – the complex set of genetic instructions we all have to develop and maintain our bodies.
“We each have a unique combination of genetic material, and with genetic sequencing now becoming more common and affordable, we can accurately identify rare diseases and determine the most appropriate treatment method,” he says.
At a glance, the human genome is a simple four-letter code: A, C, G, T. How those letters line up in an individual’s genome, however, indicates disease or potential for disease. As such, knowing how they line up is an invaluable diagnostic tool.
There are 4,800 known, rare syndromes, affecting between one and two million Canadians. More accessible gene sequencing has allowed Bernier and his colleagues to diagnose many previously undiagnosed, complex chronic diseases, which has a positive impact on families as well as the health care system.
The cost to sequence the full genome in one single person used to be $100 million, Bernier says, but like many things the cost has decreased over time. It now costs about $1,000. “It’s like buying a Ferrari for 25 cents.”
However, it's not feasible yet to screen the entire population. "These technologies are complex and introducing them into the health care system will take time," he says, “but we're fortunate that through support of the Alberta Children's Hospital Research Institute and the Cumming School of Medicine, the Centre for Health Genomic and Informatics can support our cutting-edge research."

.
Like many of us, Sharon Strachan’s exercise companion is an iPod. But Strachan’s iPod does a few things yours and mine can’t: it helps her manage the symptoms of Parkinson’s disease.
Before Strachan goes out for her daily walk, she straps her iPod on her leg, near the knee. During her walk, the music stops if she slows down too much or takes shorter steps. Once she adjusts her stride and her gait, the music begins to play again.
Strachan’s iPod uses the Gait Reminder app, developed by Bin Hu in UCalgary’s Movement Disorder Clinic in the Hotchkiss Brain Institute. A sensor in the device senses the wearer’s steps and causes the iPod to react accordingly.
“The Gait Reminder works on the principle of reward-based motivation,” explains Dr. Hu, a UCalgary professor in the Cumming School of Medicine's department of neurosciences. “To activate the brain there is a behavioural paradigm: if you make effort and succeed, you will be rewarded. And in the motivational part of the brain, music is a very strong component.”
"In the motivational part of the brain, music is a very strong component.”
Parkinson’s is a progressive nervous system disease, characterized by tremors, impaired posture and balance, and slowed movement. Many people who have Parkinson’s can have difficulty walking, with their steps becoming shorter until they eventually shuffle, or even “freeze” in place. Injuries due to falling increase with time.
Sharon Strachan says in the five years she’s used the Gait Reminder app, she’s noticed some encouraging signs. “I have no left-hand tremors anymore, can walk up the stairs OK, and can walk down the stairs using the handrail for support. I’ve had no freezing after walking to music.”
She prefers music with movement. ABBA’s Dancing Queen is one of her favourites: “It’s got life and vitality.”
Dr. Hu says the 60-song playlist the clinic provides covers the musical spectrum, from country to gospel to contemporary. The favourite? Anything by R&B and funk artist Bruno Mars.
The device that makes the music happen can connect to the clinic with Wi-Fi, sending data to co-ordinators who remotely customize the program settings to ensure patients can walk safely with optimal outcomes, says Dr. Hu.
If you have young onset Parkinson’s disease and wish to participate in the Gait Reminder/Ambuloso research program, contact:
Alec Watts
Research Assistant / Program Coordinator
Parkinson's Music Walking Program, Calgary Site
Health Research Innovation Centre (HRIC), Foothills Hospital
Cell: (403) 472-5505
Lab: (403) 220-4486
.
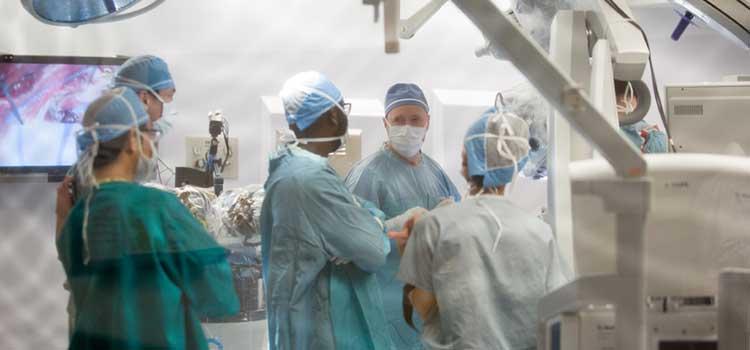
In preparing to perform an operation, surgeons mentally walk through what they must do. They visualize the necessary steps they will take to successfully perform the operation.
“Typically, a surgeon will review a pre-operative two-dimensional CT scan of the patient to prepare for the operation before going into the operating room,” says Dr. Sonny Chan, PhD, assistant professor of computer science at UCalgary's Faculty of Science. “We’ve found a way to enhance the surgery planning and rehearsal by offering a three-dimensional view of the actual patient.”
Combined with this view is the application of haptics – recreating the sense of touch. So a surgeon can actually practise the surgery and feel contact and resistive forces, with the anatomical model responding in a physically realistic manner.
One application of the tool is in temporal bone surgery – surgery of the bone that surrounds the ear canal. A surgeon could prepare for surgery to remove a tumour or insert a cochlear implant using a realistic model of the patient.
While Chan says haptics is “very cool but not cheap to produce,” surgery is one of the disciplines that can afford the cost. “We’ve had extremely good uptake in the surgical community. Regardless of their years of experience, surgeons are embracing the technology,” he says.
And while the tool is still at the research stage, Chan says there is anecdotal proof that it will have benefits at the clinical stage. “Residents are evaluated on their performance in cadaver dissection,” he explains. “The resident who uses the tool does better than someone who studies CT scans before dissection.”
.
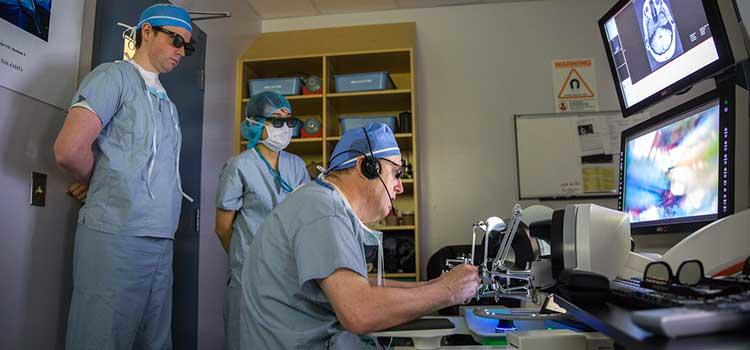
Nine years ago, Dr. Garnette Sutherland and his team made history. Dr. Sutherland, a member of the Hotchkiss Brain Institute, is a professor in the Cumming School of Medicine and an Alberta Health Services neurosurgeon. Sutherland successfully removed a brain lesion from 21-year-old Paige Nickason – using a robot. The surgery was the culmination of almost 10 years of research and development, with the goal of making surgery more precise and accurate.
The neuroArm robot works in tandem with a ceiling-mounted, movable, high-field, intra-operative magnetic resonance imaging system (iMRI) previously developed by Sutherland. This allows the surgeon to access images in real-time without disrupting the surgery to move the patient out of the OR. The robot is controlled from a sensory-immersive workstation in a room adjoining the surgical suite.
Since that groundbreaking surgery, this technology has helped more than 65 patients, while the iMRI has been used in more than 2,000 patients in Calgary and more than 20,000 around the globe. A second-generation robot has received approval from the Food and Drug Administration in the United States, and Dr. Sutherland’s team continues to refine the robot, having launched a small, economic third-generation version called CellArm.
“You can’t have a costly robot if you want to use it in healthcare."
“You can’t have a costly robot if you want to use it in healthcare,” Sutherland says. “Robotic technology, capable of performing repetitive and precise tasks, can in the long term improve the cost of healthcare in a positive way.”

Caption
– – – – –
– – – – –
Dr. Elise Fear, PhD, is a professor in electrical and computer engineering at UCalgary’s Schulich School of Engineering. Her research interests are in creating flexible sensing and imaging systems that integrate multiple, low-cost sensing technologies to provide sensitive and specific detection of targets. View Elise's publications
Dr. Bin Hu, MD, PhD, is a professor in the Cumming School of Medicine's department of neurosciences. His research interests include movement disorders, Parkinson's disease, music and wearable technology. View his publications
Dr. Sonny Chan, PhD, is an assistant professor of computer science in UCalgary's Faculty of Science. His research interests include computer haptics, medical visualization, medical image analysis, virtual environments and immersive simulation.
Dr. Garnette Sutherland, MD, is a professor in the Cumming School of Medicine, an Alberta Health Services neurosurgeon, and a member of the Hotchkiss Brain Institute. His major research focus has been the application of MR techniques to the study of neurological diseases. View Dr. Sutherland's publications
Dr. Francois Bernier, MD, is a member of the Alberta Children's Hospital Research Institute, the head of the department of medical genetics at the Cumming School of Medicine and director of the clinical genetics unit at the Alberta Children’s Hospital. View Dr. Bernier's publications